At Healing Hospital, we understand that living with Parkinson’s disease, essential tremor, dystonia, or other movement disorders significantly impacts quality of life, and concerns about brain surgery may create anxiety about treatment options—requiring advanced, precise neurosurgical solutions with proven outcomes. That is why our advanced Neurosurgery & Functional Neurosurgery Department, led by gold medallist neurosurgeons with specialized training in Deep Brain Stimulation and extensive experience in stereotactic functional neurosurgery—offers state-of-the-art Deep Brain Stimulation (DBS) surgery using advanced stereotactic navigation systems, microelectrode recording technology, intraoperative neurophysiological monitoring, and comprehensive pre and post-operative care protocols. This ensures precise electrode placement in targeted brain structures, optimal symptom control, improved quality of life, and superior long-term outcomes for patients with medication-refractory movement disorders.
We have served patients across 25 states of India—a few of them are Chandigarh, Punjab, Haryana, Himachal Pradesh, J&K, Madhya Pradesh, Bihar, Jharkhand, West Bengal, Gujarat, and many others, with our comprehensive functional neurosurgery services including DBS for Parkinson’s disease, essential tremor, dystonia, and other movement disorders, advanced stereotactic techniques, comprehensive pre-operative patient selection and counselling, expert programming and optimization of DBS systems, long-term follow-up and device management, and multidisciplinary care involving neurologists, neurosurgeons, and rehabilitation specialists. Healing Hospital’s track record reflects proven excellence ensuring optimal results with patient safety, precision, and life-transforming symptom improvement as highest priorities.
If you are searching for “best DBS surgeon in Chandigarh,” “Parkinson’s disease surgery,” “tremor treatment,” “movement disorder specialist,” or “functional neurosurgery,” you have found a centre where surgical excellence meets specialized training and cutting-edge neurosurgical expertise.
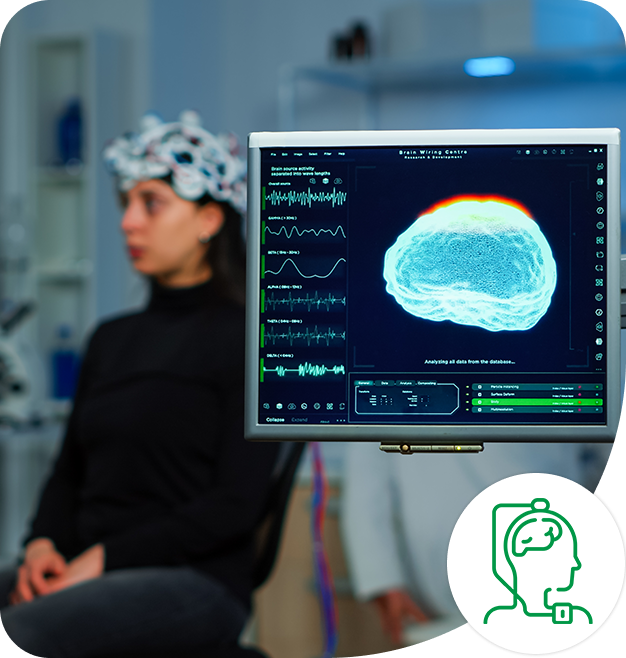
What is Deep Brain Stimulation (DBS)?
Deep Brain Stimulation (DBS) is an advanced functional neurosurgery procedure that involves surgical implantation of electrodes (thin wire leads) into specific deep brain structures, connected to a programmable neurostimulator device (similar to a cardiac pacemaker) implanted under the skin below the collarbone. The neurostimulator delivers precisely controlled electrical impulses to targeted brain regions, modulating abnormal neural activity and providing dramatic relief from movement disorder symptoms such as tremors, rigidity, slowness of movement (bradykinesia), and involuntary movements (dyskinesias).
Key Analogy: DBS works like a "pacemaker for the brain"—just as a cardiac pacemaker regulates abnormal heart rhythms with electrical impulses, DBS regulates abnormal brain activity causing movement disorder symptoms. The stimulation doesn't cure the underlying disease but provides remarkable symptom control, often reducing medication requirements by 50-70% and dramatically improving quality of life.
Schedule Your Appointment with
Our Expert Doctors
We are dedicated to driving lasting, positive transformation in healthcare management through innovation and patient-centered solutions.
Who is a Suitable Candidate for Deep Brain Stimulation?
DBS is suitable for patients with:
- Parkinson's Disease; Not getting improved with medications or showing any side effects
- Essential Tremor affecting hands, head, or voice
- Significant functional impairment - difficulty in standing, writing, eating, walking
- Dystonia - significant disability from abnormal postures and involuntary movements
What Happens Before, During, and After Deep Brain Stimulation?
Before Surgery
Comprehensive Candidate Selection & Surgical Planning
A rigorous multidisciplinary evaluation is conducted to ensure optimal outcomes, beginning with a detailed movement disorder assessment that includes a Levodopa challenge to confirm medication responsiveness and standardize motor symptoms using the UPDRS scale. This is paired with neuropsychological screening to evaluate cognitive and psychiatric stability, alongside high-resolution 3D brain imaging (MRI/CT) for precise anatomical mapping and target selection (STN vs. GPi).
During Surgery
Precision Electrode Implantation
On the day of surgery, a stereotactic frame and advanced 3D imaging are used to establish millimeter-precise target coordinates. Under conscious sedation, the patient remains awake to provide vital neurological feedback; microelectrode recording identifies the specific neuronal "signatures" of the target (STN or GPi). Clinical macrostimulation is then performed to confirm immediate symptom relief, such as tremor suppression, before the permanent quadripolar leads are secured to the skull and tunneled under the scalp.
Neurostimulator Integration
Following the brain surgery, the patient is placed under general anesthesia for the final stage of the procedure. A small subcutaneous pocket is created below the collarbone to house the Implantable Pulse Generator (IPG). Extension wires are tunneled discreetly under the skin of the neck to connect the brain electrodes to this battery-powered stimulator. This integration completes the circuit, transforming the high-precision implants into a fully programmable system ready for long-term symptom management.
After Surgery
Hospital Stay & Initial Healing
Following surgery, patients are monitored in a specialized neurosurgical ward to assess motor function and recovery. A post-operative scan (CT/MRI) confirms precise electrode placement. To allow the brain to heal from the surgical "microlesion effect," the DBS system remains inactive for the first few weeks. Patients are typically discharged within 4 days with instructions to avoid strenuous activity and keep incisions dry.
System Activation & Programming
Once the brain has recovered, the patient returns for the Initial Activation. Each electrode contact is systematically tested to find the optimal stimulation parameters. While tremor suppression is often immediate, improvements in rigidity and bradykinesia occur gradually. As the DBS effect stabilizes, Parkinson’s medications are typically reduced by 30–50%, significantly decreasing medication-related side effects.
Optimization & Long-Term Maintenance
Over the first six months, iterative programming sessions fine-tune the stimulation for maximum symptom control. Once stable settings are achieved, follow-ups transition to every 3–6 months for routine checks and medication management. The neurostimulator battery is replaced through a simple outpatient procedure every few years, ensuring sustained, long-term neurological stability.
What are the Recovery & Success Factors?
Dramatic Symptom Improvement: Parkinson's Disease
DBS provides 90-100% improvement in motor symptoms (tremor, rigidity, bradykinesia) during "off" medication states. Tremor control is excellent—often 80-90% improvement. Quality of life is significantly enhanced.
Essential Tremor
90-100% tremor reduction in most of the patients—dramatic improvement enabling functional activities (eating, writing, self-care). Immediate benefits can often be seen in the operating room when test stimulation is performed.
Dystonia
80-100% improvement in dystonia severity and functional disability. Benefit accumulates gradually over 3-6 months (unlike Parkinson's/tremor where improvement is more immediate). Quality of life significantly enhanced.
Medication Reduction & Reduced Side Effects
DBS enables 80-90% reduction in Parkinson's medications—decreasing levodopa-related dyskinesias, psychiatric side effects (hallucinations, confusion, impulse control disorders), and medication costs whilst maintaining better symptom control than medications alone achieved.
Sustained Long-Term Benefit
DBS provides sustained benefit for 10-15+ years—unlike medications where efficacy declines progressively. Studies show maintained motor improvement and quality of life enhancement lasting over decades with appropriate programming adjustments and battery replacements.
Adjustability & Reversibility
Unlike ablative procedures permanently destroying tissue, DBS is fully adjustable—stimulation parameters optimized non-invasively as disease progresses or patient needs change. Fully reversible—can be turned off if problems occur or removed if better treatments emerge.
Why Choose Healing Hospital in Chandigarh for Deep Brain Stimulation?
What are the Advantages of Deep Brain Stimulation?
Following are the key advantages of getting Deep Brain Stimulation:
- Dramatic Symptom Control
- Better Motor Skills & Reduction in Tremors
- Reduction in Dependency on Medications
- Reversible & Adjustable Treatment
- Both sides of the brain can be treated simultaneously
- Improved Quality of Life
- Long-Term Efficacy
- Minimal Cognitive Effects
What are the Risks & Complications Involved in Deep Brain Stimulation?
While DBS is a safe procedure performed worldwide for 25+ years with excellent safety profile, patients should be aware of potential risks:
Intracranial Hemorrhage (Brain Bleeding)
Most serious surgical risk—occurs in 1-2% of procedures. Small hemorrhages are usually asymptomatic; larger bleeds may cause stroke-like symptoms. Risk minimized by careful surgical technique, blood pressure control, discontinuing blood thinners pre-operatively.
Infection
Surgical site infection (scalp incision, chest pocket) or hardware infection occurs in 3-5%. Treated with antibiotics; sometimes requires hardware removal and reimplantation after infection cleared. Risk minimized by prophylactic antibiotics, meticulous sterile technique, ultra-sterile modular OT environment.
Electrode Misplacement
Rare with modern stereotactic techniques and microelectrode recording—ensuring precise targeting. If significant misplacement occurs, electrode repositioning may be needed.
Lead Fracture or Migration
Electrode wire breakage or movement over time—may require revision surgery replacing damaged lead.
Erosion
Hardware eroding through skin (scalp or chest)—requires surgical revision repositioning hardware.
Battery Replacement Needed
Non-rechargeable batteries last 3-5 years; rechargeable systems 15+ years. Battery replacement is a simple outpatient procedure under local anaesthesia.
Blog
Frequently Asked Questions (FAQs)
What makes Deep Brain Stimulation different from medications and ablative procedures?
Deep Brain Stimulation is reversible, adjustable, and bilateral-safe—three crucial advantages. Unlike medications that lose efficacy over time and cause increasing side effects, DBS provides sustained symptom control for 10-15+ years whilst enabling 80-90% medication reduction. DBS is safe for both brain sides simultaneously providing symmetric symptom control, whilst bilateral lesioning carries high risk of speech and swallowing problems.
How soon will I see improvement after DBS surgery?
Tremor improvement is often immediate—dramatic tremor suppression visible within seconds of test stimulation during surgery, sustained once DBS activated 2-4 weeks post-op. Rigidity and bradykinesia improve gradually—50-70% better within days of activation, full benefit over 1-3 months as optimal programming is achieved and medications adjusted. Dyskinesias reduced once medications decreased (happens over weeks to months). Dystonia improves slowly—benefit accumulates gradually over 3-6 months, reaching maximum by 6-12 months.
How long do DBS results last?
DBS provides sustained benefit for 10-15+ years based on long-term studies following patients for over a decade. Studies show maintained 90-100%% motor symptom improvement and quality of life enhancement lasting over decades with appropriate programming adjustments. Unlike medications where efficacy progressively declines, DBS benefit remains stable. Battery replacements are 15+ years (rechargeable), but the benefit continues indefinitely.
Will I still need to take medications after DBS?
A few patients with excellent DBS response reduce medications further; while others discontinue completely (rare). The goal is optimal symptom control with minimal medication side effects—not necessarily medication elimination.
Is Deep Brain Stimulation reversible if I have problems?
Yes, completely reversible. If problems occur, DBS can be turned off immediately using an external programmer—effects reverse within hours as stimulation stops. Electrodes can be surgically removed if necessary (though rarely needed). This reversibility is a major advantage over ablative procedures where tissue destruction is permanent.
Can DBS be done on both sides of the brain?
Yes, bilateral DBS is standard for Parkinson’s disease and generalized dystonia—both sides treated in the same surgery providing symmetric symptom control. Bilateral DBS is safe with modern techniques and targets (STN or GPi). This is a major advantage over ablative lesioning where bilateral procedures carry high risk of speech, swallowing, and cognitive problems. For essential tremor, bilateral DBS performed simultaneously or staged depending on symptom distribution and patient preference.
How much does Deep Brain Stimulation surgery cost in Chandigarh?
Contact us at +91-7986115995 for detailed transparent pricing. Cost includes comprehensive package: pre-operative multidisciplinary evaluation (movement disorder neurologist, neurosurgeon, neuropsychologist), brain MRI and surgical planning, stereotactic DBS surgery with microelectrode recording (bilateral), neurostimulator implantation, hospital stay and post-operative monitoring, initial DBS activation and programming sessions, follow-up care.
How do I schedule a Deep Brain Stimulation consultation?
Contact our Neurosurgery Department at +91-7986115995 to schedule consultation with our functional neurosurgery team. Please bring: complete medical records documenting movement disorder diagnosis and progression, list of all medications tried with doses and responses, current medication regimen, recent brain MRI (if available), previous neurologist evaluations, and your questions. Consultation includes comprehensive movement disorder assessment by our team, detailed discussion of DBS candidacy, realistic outcome expectations based on your specific condition, explanation of surgery and programming process, and multidisciplinary evaluation recommendations.